Treatment of murine autoimmune myocarditis with a novel monoclonal antibody that targets multiple inflammatory pathways
Treatment of murine autoimmune myocarditis with a novel monoclonal antibody that targets multiple inflammatory pathways
Toldo, S.; Luger, D.; Vozenilek, A.; Abbate, A.; Kelly, J.; Mezzaroma, E.; Shibao, C. A.; Abd-ElDayem, M. A.; Klenerman, P.; Waksman, R.; Virmani, R.; Maynard, J. A.; Harrison, D.; Flugelman, M. Y.; Epstein, S. E.
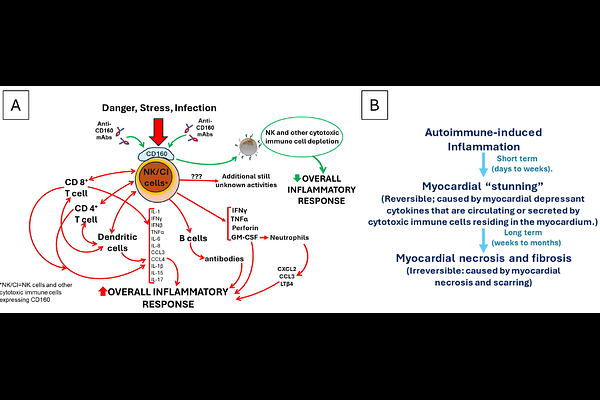
AbstractAbstract: Severe forms of inflammation-induced acute and chronic myocarditis have a poor prognosis. Promising therapeutic efforts focused on monoclonal antibodies (mAbs) inhibiting inflammation-inducing molecules. However, most mAbs target only one or a limited number of such molecules. Since inflammation involves multiple redundant pathways, we postulated that an mAb inhibiting multiple inflammatory pathways would be a potent therapeutic agent. We initially tested the commercially available anti-natural killer (NK) cell mAb (anti-NK1.1), which binds a receptor expressed on NK cells and depletes them. Since NK cells are key cellular orchestrators of inflammation, by reducing their number, we aimed to inhibit multiple inflammatory pathways. Our initial studies demonstrated that administration of this antibody significantly improved myocardial outcomes in mouse models of acute myocardial infarction and of heart failure. Since NK1.1 is not expressed in human cells, we built on these promising preclinical results by developing a novel mAb targeting CD160 on human NK cells for evaluation as an immunosuppressive therapy. We found that the anti-CD160 mAb depletes both murine and human NK cells. We also found that, while CD160+ cells were largely present in the NK population, they also occurred among CD8+ and {gamma}/{delta} T cell subsets in human cells. Anti-CD160 therapy entirely prevented the deterioration of the myocardial function of mice with autoimmune-induced acute myocarditis. This outcome suggests our novel approach for inhibiting multiple inflammatory pathways may provide a potent strategy for improving outcomes of inflammation-driven myocarditis, as well as of other inflammation-driven diseases.