Intranasal Anti-CD3 Antibody Treatment Attenuates Post-COVID Neuroinflammation and Enhances Hippocampal Neurogenesis and Cognitive Function in Mice
Intranasal Anti-CD3 Antibody Treatment Attenuates Post-COVID Neuroinflammation and Enhances Hippocampal Neurogenesis and Cognitive Function in Mice
Lu, P.; Izzy, S.; Da Silva, P.; Imkamp, H. T.; Christenson, J. R.; Yahya, T.; Mansi, M. H. A.; Alawi, A.; Moreira, T. G.; Monje, M.; Weiner, H. L.; Iwasaki, A.
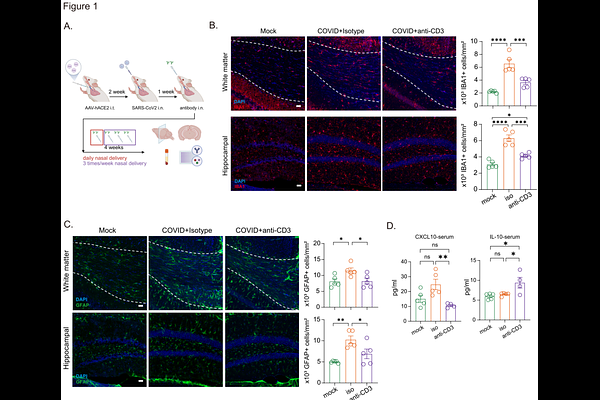
AbstractCognitive impairment is a disabling feature of Long COVID, with data supporting neuroinflammation and maladaptive glial responses as primary drivers. Nasal administration of an anti-CD3 monoclonal antibody (aCD3 mAb) has shown therapeutic benefits in autoimmune and CNS disease models. Using a respiratory-restricted mild SARS-CoV-2 mouse model of Long COVID, we show that nasal anti-CD3 mAb, administered shortly after infection or during chronic neuroinflammation, increased brain FoxP3+ IL-10+ Tregs, reduced microglial and astrocytic gliosis in the white matter and hippocampus, restored neurogenesis, and improved short-term memory. Nasal aCD3 mAb reprogrammed microglia from an antigen-presenting, NF-{kappa}B-driven inflammatory state toward chemokine signaling, phagosome, and TGF{beta}-related regulatory phenotype. Patients with Long COVID with neurological symptoms had lower circulating Treg populations. These findings identify nasal administration of aCD3 mAb as a noninvasive strategy to control neuroinflammation, restore the neurogenic niche, and offer a novel approach to treating cognitive impairment in Long COVID.