Impairing NK-mediated immune rejection through NKG2DL editing to improve CAR-T cell persistence
Impairing NK-mediated immune rejection through NKG2DL editing to improve CAR-T cell persistence
Shi, H.; Wang, Y.; Tang, X.; Liu, G.
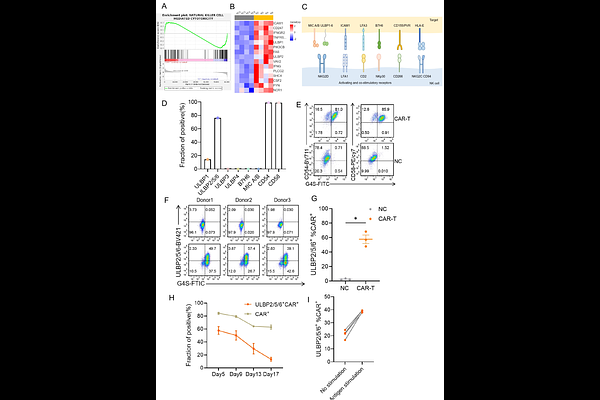
AbstractCAR-T immunotherapy has achieved remarkable efficacy in hematologic malignancies. However, the widespread clinical adoption of autologous CAR-T products remains constrained by high costs, lengthy manufacturing process, and limited accessibility. Universal or off the shelf CAR-T (UCAR-T) cells derived from healthy donors offer a promising alternative, enabling immediate treatment at a lower cost. However, the allogeneic nature of UCAR-T cells triggers immune rejection by the host immune system after infusion, thereby compromising their persistence and therapeutic efficacy. Current strategies to circumvent this rejection focus on disrupting HLA class I expression. Although this modification allows UCAR-T cells to successfully evade T cell mediated elimination, the loss of HLA class I molecules renders them vulnerable to attack by host natural killer (NK) cells. In contrast to previous approaches that attempt to retain certain non-classical HLA molecules (such as HLA-E or HLA-G) to inhibit NK cells, we directly focused on editing the ligands that mediate NK cell rejection. Through transcriptomic and in vitro validation analyses, we found that UL16 binding proteins (ULBP) 2/5/6 were substantially upregulated in UCAR-T cells compared with nontransduced donor T cells. Elevated ULBP expression effectively activates the NKG2D receptor on allogeneic NK cells and leads to killing of UCAR-T cells, thereby impairing UCAR-T function. To test whether abrogating this NK activating signal could improve UCAR-T persistence and antitumor efficacy, we generated ULBP knockout UCAR-T cells using CRISPR-Cas9 editing. Deletion of ULBP2/5/6 significantly reduced NK cell mediated killing in vitro without affecting CAR expression or T cell effector function. Compared with wild type UCAR-T cells, ULBP deficient UCAR-T cells exhibited enhanced tumor killing efficacy in the presence of NK cells. Collectively, our findings identify ULBP upregulation as one of the mechanisms underlying NK cell mediated rejection of HLA deficient UCAR-T cells. Targeted ablation of ULBP molecules provides a novel strategy to confer resistance to host NK cells, thereby improving the therapeutic potential of universal CAR T products.